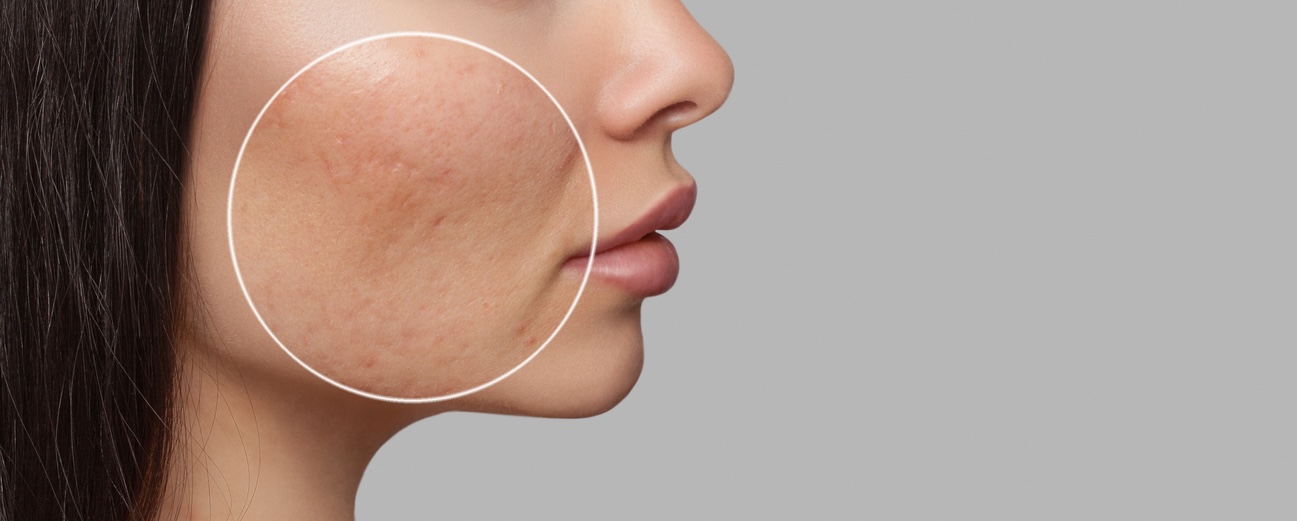
Q: What is Rosacea?
Rosacea is a chronic inflammatory condition of the skin that typically begins when superficial blood vessels in the face dilate too easily and cause central facial redness. Over time, the redness “builds up” and gives the skin a persistent sunburned, ruddy appearance. In addition to redness, patients may develop acne like bumps and pustules, thickening of the skin (particularly on the nose), and eye irritation. Rosacea most commonly impacts fair complected adults after age 30, particularly those with a history of facial flushing.
Q: What Causes Rosacea?
While we don’t know the underlying cause of rosacea, we know quite a bit about its triggers and contributing factors. When I counsel patients on lifestyle factors that trigger rosacea flares, I’ve been asked more than once if rosacea is caused by “all the good stuff.” Sun, exercise, a spicy meal, stress, cold weather, and alcohol top the rosacea trigger list and can make rosacea feel like the vengeful enemy of fun. But why can your girlfriend enjoy a margarita and spicy salsa and stay looking cool and calm while you look like a chili pepper? On a basic level, the face turns red when the superficial blood vessels dilate, aka “vasodilation”, and in the setting of rosacea, this happens too easily. It is thought that in patients with rosacea there is a complicated interplay between the innate immune system, harmless microbes living in the skin, neurovascular responses, and genetics that leads to the inflammatory vasodilatory response. Rosacea treatments target those various factors, and along with lifestyle modifications can be very effective in controlling rosacea.
Q: Is There a Connection Between Rosacea and Other Skin Conditions?
Seborrheic dermatitis and perioral dermatitis are common skin conditions that are often seen alongside rosacea. They may share pathways regarding overgrowth of microorganisms and the inflammatory response, and they often respond to rosacea treatments. It is important to note that Lupus is a condition that presents similarly to rosacea with midfacial redness, but patients with rosacea are not at higher risk for developing Lupus. A Dermatologist can help differentiate between lupus and rosacea and direct treatment appropriately.
Q: Can Rosacea Be Diagnosed Before a Flare Up?
There are some early signs that a patient may have rosacea before it truly declares itself. One of those is prolonged flushing starting in the teens or twenties, often accompanying acne-like break outs. Another tip off that a patient may have early rosacea is when the acne treatments are causing excessive irritation and worsening the break outs. A history of sensitivity and irritation to multiple skin care products, even gentle ones, is another clue that a person may have early rosacea.
Q: How Long After a Trigger Will a Rosacea Flare Up Occur?
This totally depends on the patient and the trigger. Some patients feel and see the flush within minutes of the trigger while others may not see the repercussions until the next day. When possible, I recommend that patients maintain awareness of rising facial heat and redness, identify the trigger if possible, and reduce that exposure.
Q: How Can Diet Affect Rosacea?
There are foods and beverages that can worsen rosacea, and there are foods that may actually help. Keep reading for tips on what to avoid and what to add — studies have shown that the appropriate dietary modifications can significantly reduce rosacea flare ups and symptoms.
Q: What Foods Should You Avoid if You Have Rosacea?
There are 4 different groups of foods to consider avoiding if you rosacea, according to research done by Dr. Rajani Katta, a diet and rosacea expert. Alcohol, heat-related (coffee, tea), capsaicin-related (peppers, spicy foods), and cinnamaldehyde-related (tomatoes, citrus, chocolate, and cinnamon). These are very different foods but they all have one thing in common — they promote dilation of blood vessels. When safe and appropriate for you nutrition needs, eliminating these food groups for 6 weeks and then adding them back in one at a time may help you better pinpoint foods to avoid and foods to continue enjoying.
Q: Are There Certain Foods You Recommend for Improving Rosacea?
Food recommendations to promote skin health and reduce inflammation are fairly consistent across many conditions and it all comes down to a better balanced gut. We have a delicate balance of good and bad microbes in our gut, and when we don’t feed the good, the bad can get ugly. We nourish the good with Prebiotics such as fruits and veggies like asparagus, artichokes, bananas, berries, whole grains, nuts and seeds, and garlic. There is also a role for Probiotics, which are live microorganisms ingested in food or supplements to help repopulate your gut with the good microbes. Yogurt, kefir, kombucha, pickled veggies, tempeh (soy), and vinegar are good dietary sources of probiotics. The best option is to combine a diet rich in prebiotics and probiotics – after all, you need to give the probiotics the nutrients needed for them to survive and thrive.
Q: How is Rosacea Treated?
Rosacea treatments are as varied as the patients they treat and need to be designed to match the symptoms. Redness can improve with multiple modalities including laser treatments, topical vasoconstrictors, and skin care targeting barrier repair. The red papules and pustules often respond to topical anti-microbial agents targeting Demodex mite and Staph epidermidis. Low-dose oral antibiotics at anti-inflammatory dosing can be very beneficial in the midst of significant and persistent flares. Very importantly, the impaired skin barrier function needs to be addressed with a skin care regimen that repairs, restores, and protects. Daily broad spectrum sun protection of SPF 30 or above is critical to improve the success of the overall treatment plan.